Nighttime sounds disrupting your sleep—or your partner’s—might seem like a harmless annoyance, but they could be signaling something more serious. While snoring affects millions of people and often poses no significant health risks, sleep apnea represents a potentially dangerous medical condition that demands attention. Understanding the difference between simple snoring and sleep apnea can be crucial for protecting your long-term health and quality of life.
Understanding Simple Snoring
Snoring occurs when air flows past relaxed tissues in your throat, causing them to vibrate during breathing. This creates the familiar rumbling or rattling sound that can range from soft and occasional to loud and persistent. The condition affects people of all ages, though it becomes more common as we get older and throat muscles naturally lose tone.
Several factors contribute to everyday snoring. Sleeping position plays a significant role, with back-sleeping often increasing the likelihood of snoring as gravity pulls throat tissues backward. Nasal congestion from allergies, colds, or sinus issues can force mouth breathing and increase snoring intensity. Alcohol consumption before bed relaxes throat muscles excessively, while being overweight adds tissue around the neck that can narrow airways.
For many people, simple snoring represents nothing more than a social inconvenience. It doesn’t interrupt their own sleep or cause daytime symptoms. While it might frustrate bed partners, it doesn’t carry the serious health implications associated with sleep apnea.
What Makes Sleep Apnea Different
Sleep apnea transforms snoring from a nuisance into a medical emergency happening repeatedly throughout the night. This condition involves actual pauses in breathing that can last seconds or even longer, occurring dozens or hundreds of times each night. Your brain must repeatedly rouse you from deep sleep to restart breathing, even though you typically won’t remember these micro-awakenings.
The most common form, obstructive sleep apnea, happens when throat muscles relax enough to block your airway completely. Each breathing pause reduces oxygen levels in your blood, forcing your cardiovascular system to work harder. Over time, this nightly stress takes a serious toll on your body.
Central sleep apnea, a less common variant, occurs when your brain fails to send proper signals to breathing muscles. Some people experience complex sleep apnea, which combines both obstructive and central elements.
Warning Signs That Point to Sleep Apnea
Distinguishing between harmless snoring and sleep apnea requires attention to specific symptoms that go beyond nighttime noise. Witnessed breathing pauses represent the most telling sign—if your partner reports that you stop breathing, gasp, or choke during sleep, sleep apnea becomes highly likely.
Morning headaches that fade as the day progresses suggest oxygen deprivation during the night. Waking with a dry mouth or sore throat indicates you’ve been breathing heavily through your mouth as you struggle for air. Excessive daytime sleepiness that persists despite spending adequate time in bed points toward disrupted sleep architecture caused by repeated awakenings.
Difficulty concentrating, memory problems, and mood changes, including depression or irritability, can all stem from the fragmented sleep that sleep apnea causes. Some people experience nighttime sweating or frequent urination as their body responds to the stress of interrupted breathing.
High blood pressure that proves difficult to control with medication may actually have sleep apnea as an underlying cause. The condition forces your cardiovascular system into overdrive night after night, contributing to hypertension even in people who otherwise maintain healthy lifestyles.
The Health Risks of Untreated Sleep Apnea
Sleep apnea’s impact extends far beyond poor sleep quality. The condition significantly increases your risk for cardiovascular problems including heart attack, stroke, and irregular heartbeat. Repeated drops in blood oxygen levels strain your heart and blood vessels, while the constant release of stress hormones damages your cardiovascular system over time.
Type 2 diabetes risk rises with sleep apnea, partly because sleep deprivation affects how your body processes glucose. Metabolic syndrome, a cluster of conditions including high blood pressure, abnormal cholesterol levels, and increased waist circumference, occurs more frequently in people with untreated sleep apnea.
Daytime fatigue from sleep apnea increases accident risk, whether you’re driving, operating machinery, or simply navigating daily activities. The cognitive impairment rivals that of alcohol intoxication in some cases, making even routine tasks potentially dangerous.
Liver problems, including fatty liver disease and abnormal liver function tests, show up more often in sleep apnea patients. The condition can also complicate surgeries and the use of certain medications, making it essential that healthcare providers know about your diagnosis.
When to Seek Medical Evaluation
Consulting an ear, nose & throat doctor or sleep specialist becomes important when snoring accompanies other concerning symptoms. If your bed partner witnesses breathing pauses, if you wake gasping or choking, or if excessive daytime sleepiness interferes with your normal activities, professional evaluation is warranted. An ear, nose & throat doctor can examine your airways for physical abnormalities that might contribute to breathing problems during sleep and recommend appropriate diagnostic testing or treatment options.
Don’t wait until symptoms become severe. Early intervention prevents the long-term health complications associated with untreated sleep apnea while improving your immediate quality of life. Many people live with undiagnosed sleep apnea for years, attributing their fatigue and other symptoms to aging, stress, or busy lifestyles when a treatable medical condition is actually responsible.
Diagnostic Approaches
Proper diagnosis typically involves a sleep study, either conducted in a specialized sleep center or through a home sleep test. These studies monitor your breathing patterns, oxygen levels, heart rate, and other vital signs throughout the night, providing clear evidence of whether sleep apnea is present and how severe it might be.
The data collected reveals how often your breathing stops, how long pauses last, and how dramatically your oxygen levels drop. This information guides treatment decisions and helps establish a baseline for measuring improvement once treatment begins.
Treatment Options That Work
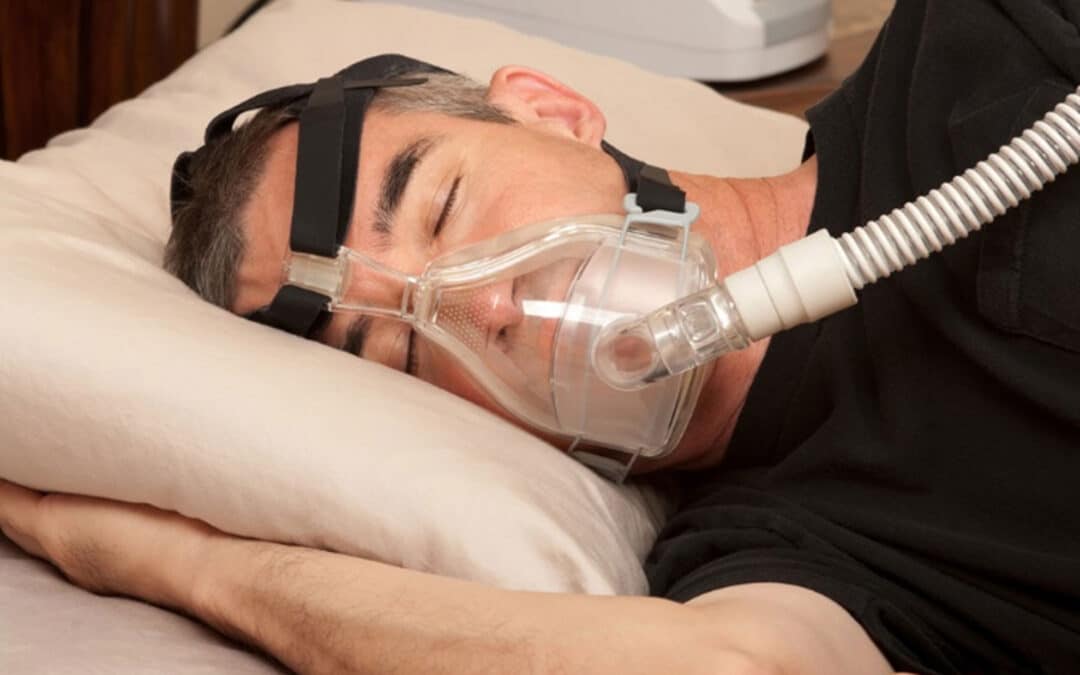
Treatment approaches vary based on sleep apnea severity and individual circumstances. Continuous positive airway pressure therapy remains the gold standard for moderate to severe cases, using gentle air pressure to keep airways open throughout the night. While adjustment takes time, most people experience dramatic improvement in symptoms once they adapt to the equipment.
Oral appliances that reposition the jaw and tongue to maintain airway opening during sleep offer an alternative for some patients, particularly those with mild to moderate sleep apnea. Lifestyle modifications, including weight loss, position training to avoid back-sleeping, and avoiding alcohol before bed, can significantly reduce symptoms in many cases.
Surgical options address specific anatomical issues that contribute to airway obstruction. These procedures range from relatively minor interventions to more extensive reconstructions, depending on what’s causing the problem.
Taking the Next Step
The difference between simple snoring and sleep apnea isn’t always obvious, but the health implications make proper diagnosis essential. If you or your loved ones have concerns about nighttime breathing patterns, daytime fatigue, or other warning signs, don’t wait to seek answers.
Our experienced team specializes in evaluating and treating sleep-related breathing disorders. We offer comprehensive assessments to determine whether your symptoms indicate simple snoring or sleep apnea, and we’ll work with you to develop a personalized treatment plan that fits your lifestyle and addresses your specific needs.
Schedule a consultation today to discuss your symptoms and explore your options. Early intervention can prevent serious health complications while restoring the restful sleep you deserve. Contact our office to book your appointment and take the first step toward better sleep and improved overall health. Your journey to quieter nights and more energized days starts with a single phone call.
Frequently Asked Questions
Can losing weight cure sleep apnea?
Weight loss often dramatically improves sleep apnea symptoms and may resolve the condition entirely in some cases, particularly when excess weight contributed to its development. However, thin people can also have sleep apnea, and weight loss alone doesn’t work for everyone.
Is sleep apnea hereditary?
Genetic factors influence sleep apnea risk through inherited traits like facial structure, airway anatomy, and body weight regulation. Family history increases your likelihood of developing the condition, though lifestyle factors also play important roles.
Will sleep apnea go away on its own?
Sleep apnea rarely resolves without intervention. The condition typically worsens over time as age-related changes affect throat muscle tone and other factors. Treatment remains necessary for managing symptoms and preventing complications.
Can children have sleep apnea?
Children definitely can develop sleep apnea, often due to enlarged tonsils or adenoids. Symptoms may differ from adult presentation, including hyperactivity, behavioral problems, and poor school performance rather than obvious daytime sleepiness.
Does snoring always mean sleep apnea?
No—many people snore without having sleep apnea. The key difference lies in whether breathing actually stops and whether you experience daytime symptoms indicating disrupted sleep quality.